Diabetic Foot Care in Chicago, IL
Diabetes results when your body fails to produce or properly use insulin
Diabetic Foot Care in Chicago & Gurnee
Two conditions can be the culprit for the loss of sensation in your feet and an increased risk of diabetic foot damage. The first is peripheral neuropathy. This disorder impacts between 60 and 70% of diabetics, and it affects what is known as the peripheral nerves in your extremities.
Peripheral neuropathy is responsible for the loss of sensation in your feet. It usually starts with strange sensations, tingling, and numbness. The good news is that if you catch it early, you and your doctor can manage it and prevent it from causing debilitating pain. Peripheral vascular disease is the other disorder that typically causes foot issues in people with diabetes.
This condition affects the arteries and veins and is characterized by a buildup of fat within your blood vessels. The most common type, peripheral arterial disease, occurs in the heart, brain, and leg and foot vessels. It puts you at risk of heart attack and stroke, and when it occurs in your legs and feet it can cause pain, discoloration, and even gangrene.
Why Does Diabetes Cause Foot Problems?
Having diabetes puts you at risk for certain conditions, like loss of sensation, poor blood flow, and nerve damage, which is especially common in the lower legs and feet. When you can't feel pain in your feet, you're unaware of any cuts, blisters, splinters, or other problems that might occur. If these problems go untreated, they can lead to foot ulcers, which require a podiatrist to treat. In the worst-case scenario, they can even lead to amputation of a toe or more. This sounds like an extreme measure, but it's to prevent infection from spreading.
Two conditions can be the culprit for the loss of sensation in your feet and an increased risk of diabetic foot damage. The first is peripheral neuropathy. This disorder impacts between 60 and 70% of diabetics, and it affects what is known as the peripheral nerves in your extremities. Peripheral neuropathy is responsible for the loss of sensation in your feet. It usually starts with strange sensations, tingling, and numbness. The good news is that if you catch it early, you and your doctor can manage it and prevent it from causing debilitating pain. Peripheral vascular disease is the other disorder that typically causes foot issues in people with diabetes. This condition affects the arteries and veins and is characterized by a buildup of fat within your blood vessels. The most common type, peripheral arterial disease, occurs in the heart, brain, and leg and foot vessels. It puts you at risk of heart attack and stroke, and when it occurs in your legs and feet it can cause pain, discoloration, and even gangrene.
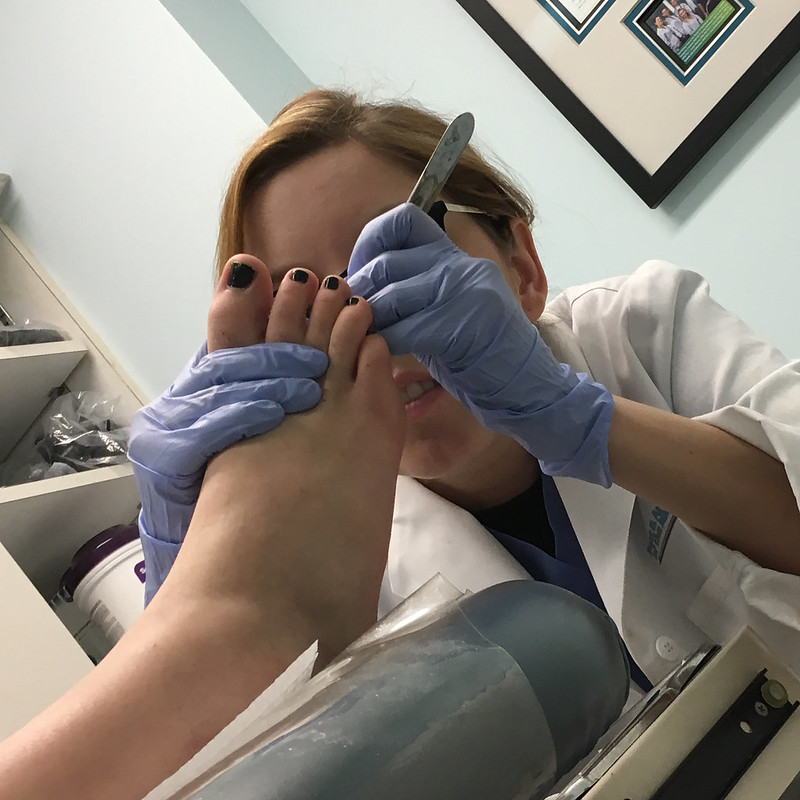
Image by woodleywonderworks is licensed with CC BY 2.0
What Are the Risk Factors?
While all people with diabetes should take good care of their feet, certain factors put them at a higher risk of developing nerve damage. You could be at increased risk of nerve damage if you have a hard time controlling your blood sugar, are overweight, are over the age of 40, have high cholesterol or blood pressure, or have had diabetes for a long time.
How Can You Care For Your Feet?
Preventing ulcers starts at home. Follow these simple tips to ensure your feet stay healthy and so that you know when it's time for a visit to the podiatrist:
- Check your feet: Choose a time every day to give your feet a visual inspection. Look for cuts, blisters, red spots, or small ulcers. If you can't see your entire foot, grab a hand mirror to get a look at the bottom.
- Wear shoes and socks: To protect your feet from hazards, always wear a pair of well-fitting shoes and comfortable socks. Even indoors, you should wear a pair of slippers so you don't accidentally step on something.
- Always change socks: Change your socks every day, and only wear socks that are in good condition. Avoid socks with holes.
- Feel inside your shoes: Make sure there are no sharp objects, like pieces of gravel or splinters, in your shoes before you put them on. If you have little or no sensation in your feet, you could walk on debris all day without being aware of it.
- Be careful cutting your nails: Cut your toenails straight across to avoid creating ingrown nails. Be careful with the nail clippers, and don't cut your skin. If you can't cut your toenails yourself, your podiatrist can help.
- Don't treat calluses at home: It's tempting to try to shave your calluses or treat them with over-the-counter patches, but avoid these measures. You could accidentally do damage to the skin of your feet. Let your podiatrist treat your calluses.
- Make a schedule with your podiatrist: Part of diabetic foot care is seeing your podiatrist regularly, especially if you've lost sensation in your feet. Discuss how often you should come in, make a schedule, and stick to it.
What Else Can You Do?
- Manage your blood sugar: Blood sugar that's frequently above target levels can put you at increased risk of neuropathy.
- Keep to a healthy diet: Focus on lean protein, low carbs, and low sugar.
- Don't smoke: Smoking is bad for blood flow and can hamper the blood's ability to transport oxygen via the blood.
What Are the Warning Signs?
Look out for warning signs that problems are developing and see your podiatrist immediately if you experience any issues. Pay attention to any tingling, burning, or loss of sensation in your feet. Warning signs might also manifest as an inability to feel temperature differences. If you notice that your legs cramp up or hurt more than they used to when you're doing something physical, that can also be a sign something is wrong.
If the way your feet look changes, that's another clue it's time to go to the doctor. Alteration in the shape, color, or temperature of your feet is something to watch for. Pay attention to whether you've lost hair on your toes, feet, or lower legs. See if the skin on your feet is dry and cracked, or if you have calluses or corns. Athlete's foot or yellowing, thickened toenails are also a cause for concern. Finally, blisters, cuts, open sores, or ingrown toenails mean you should make a podiatrist appointment immediately.
We know people with diabetes have a lot to pay attention to already, and we would hate to see a preventable foot problem become a serious issue. Whether you were recently diagnosed or you've had diabetes for years, your feet deserve the best of care. If you're having any of the problems described above, or you need to find a Chicago podiatrist to help with diabetic foot care, give Dr. Lisa Schoene a call.
If a diabetic patient develops a wound or ulcer, it is important to evaluate and treat the ulcer immediately and treat it with regular visits at the office. This will include cutting edge wound care treatments, and shoe gear considerations in order for the wound to be off loaded and heal properly.
"Excellent, thorough explanation of everything. Very friendly and approachable." "Just waiting for blood test results. Dr. Schoene took so much time with us at our first visit. She was very thorough. Never felt like she was rushing us out!"
- N.D.
Peripheral Neuropathy
Peripheral neuropathy is a disorder the affects the peripheral small nerves within the feet and legs and even the hands. These nerves exit out of the spinal cord and then enter into to muscles, and skin of the legs feet and hands, and even can affect the internal organs.
Although Neuropathy affects the diabetic population at a very accelerated rate (approximately 60-70% of all diabetics will develop neuropathy) it can affect other patients as well. Those patients may have a history of significant alcohol use, B vitamin deficiencies, and even autoimmune disorders, trauma, toxins, thyroid and lower back conditions.
Some neuropathy issues are caused by unknown factors. Usually affecting the hands and feet, peripheral neuropathy can cause, numbness, tingling, burning, and unusual sensations or pain.
Early on, it can come and go, slowly progress, or can become severe and debilitating. If diagnosed early, peripheral neuropathy can often be controlled, or even cured. Therapy is directed to treat the underlying cause and to improve the symptoms.
Peripheral Vascular Disease (PVD)
Peripheral vascular disease (PVD) can affect the arteries and veins. The most common type is peripheral arterial disease, or PAD.
It is caused by a build-up of fatty material within the vessels, called atherosclerosis. Known to affect the arteries of the heart, brain, and smaller leg and foot arteries.
If the blockage plaque breaks loose it may travel into other arteries and may cause heart attack, or stroke. If the plaque continually builds up, ischemic pain, cold feet, bluish skin discolorations, or gangrene can occur in the lower extremity.
A simple vascular check of the extremities by a professional is very important and can help diagnose this disease early.
If further diagnostic testing is required, it can usually be done painlessly and easily. By age 65, about 12 to 20 percent of the population will have this artery disease and if the patient smokes, has diabetes, hypertension, or high cholesterol, the odds increases many fold.
Simple diet changes, exercise and cessation of smoking, can greatly reduce the odds of complications of this preventable disease.
" I was made to feel very welcome when I came for my first appointment . The staff is so friendly and compassionate. Dr. B was GREAT!
- M.M.

She always keeps in mind the movements of each sport and incorporates that into the treatment plan.

